Varicose vein research laboratory
February 19, 2026
A 38 year-old man presented with symptoms of aching, burning, severe cramps and a feeling of bursting of his right leg when any attempt was made to walk briskly or climb stairs. He also complained that he was finding it increasingly difficult to lift his leg clear of the stair tread.
In 2001 he sustained an injury to his right thigh when attempting to cut a piece of meat in his kitchen. The knife he was using slipped and plunged into his thigh about half way down. Simple first aid was administered and the wound healed but he noticed that his leg started to swell and this became progressively worse as time went on.
In 2011 he consulted a vascular surgeon who diagnosed an arterio-venous fistula (AVF) between the femoral artery and vein in the mid-thigh. An AVF is an abnormal communication between an artery and a vein and one of the commonest causes is trauma where both vessels are injured and when they heal they join together to establish abnormal flow. The blood in the artery is meant to travel on down the leg to the foot but a certain amount of it was now diverting back up the vein leading to a so-called ‘steal’ syndrome.
This is demonstrated in diagrammatic form in the picture. Picture A shows when the knife injury occurs; there is a lot of bleeding between the vessels and a clot forms. As this is broken down during healing, because there are holes in the artery and vein and they are next to each other blood starts to flow out of the artery into the vein so less gets to the distal parts and a fistula forms (B). In picture C, the fistula is well established and the wall of the vein gets thicker damaged because of the excess pressure.
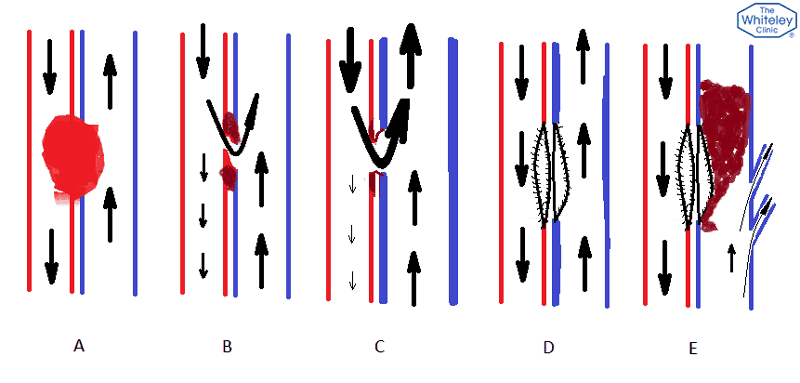
The surgeon who saw him explained that preferably a tube stent is placed in the artery at the site of the hole to prevent the blood passing out through it but that the hole was too big and an open operation would be necessary. The surgeon used a superficial vein to repair the holes in the artery and vein and all appeared to go well. However, in the intervening period the leg has become heavier and more uncomfortable with the symptoms described above. Marching the man up and down the corridor in the clinic soon produced the bursting sensation and a clear limp. The symptoms were classic for venous obstruction and so I arranged a scan to confirm my suspicions. Sure enough the scan revealed a 4 cm blockage in the femoral vein which I suspect occurred not long after the repair of the AVF.
The artery was flowing fine but arteries have a fast high pressure flow that is more likely to keep the repair open but veins are slower and much lower pressured and small clots can easily form along the repair edges leading to a complete block which if it becomes established leads to congestion in the lower part of the leg and foot resulting in the bursting feeling experienced by this young man. D shows the situation after the surgical repair; all would appear to be well but thickening of the vein wall and the tendency for blood particles to adhere to the join in the repair patch leads to thrombosis and scarring and finally occlusion as shown in picture E. There is an attempt to bypass round the block or collateralise but because the occlusion happens relatively quickly there is little time to form collateral veins and they prove inadequate. Whilst there are risks, there is a possibility of opening up the block and placing a stent across the damaged area; technology and expertise have improved considerably in recent years and hopefully this man can be helped.
Kind regards, Barrie Price