Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Compression stockings are commonly used for varicose veins, but it is important to know that they are not a cure. Recent research suggests a different approach to treating varicose veins. In an article on the Daily Mail website, Professor Mark Whiteley explains that compression stockings offer some relief from symptoms, and may even help in people unable ot have other definitive procedures. However, they should not replace proper medical treatments. Updated guidelines from the National Institute for Health and Care Excellence (NICE) recommend more effective procedures to treat varicose veins. These include Endovenous Laser Ablation (EVLA), Radiofrequency Ablation (RFA), and as a second best to these, Foam Sclerotherapy.
Varicose veins are very common. They can affect about 40% of women and 25% of men. When visible on the surface, these veins often look swollen, twisted, and can ache or cause “heavy” or “tired” legs. They usually appear on the legs and ankles. However, there are also “hidden varicose veins” - these are the same condition but without anything visible on the surface. These are more worrying, as they can go on to cause all of the same problems that untreated varicose veins can cause, but without showing on the surface.
Varicose veins form when the walls of the veins become weak due to altered flow inside the veins. As a result, the veins swell and lose their shape. Normally, veins in the legs push blood back from the feet to the heart. They work hard because they must fight against gravity. Inside each vein, there are tiny one-way valves. These valves help keep the blood moving in the right direction. However, when varicose veins occur, the vein walls weaken, and the valves cannot close properly anymore. We do not know if the valves fail, causing the walls to stretch, or if the walls stretch, stopping the valves from closing properly. Whichever comes first, the result is that blood falls back down the veins with gravity, “venous reflux” and it pools inside the veins, leading to a condition called "venous stasis." Over time, the combination of refluxing and pooled blood causes veins to stretch and push outwards under the skin. This pressure can irritate nearby nerves, and both venous reflux and stasis cause inflammation in the lower leg. Common symptoms include heavy legs, tiredness, burning sensations, and throbbing pain. If the varicose veins or hidden varicose veins are not treated, this inflammation can damage the tissues of the lower leg, resulting in eczema, red or brown stains, blood clots, bleeding, or leg ulcers (open sores).
Compression stockings have been a standard treatment for varicose veins for over fifty years. However, recent studies indicate that they have limited effectiveness. They only help temporarily improve symptoms. The National Institute for Health and Care Excellence (NICE) now advises against using them as the first-line treatment. These stockings are designed to be tight around the ankle. Moreover, they gradually loosen towards the knee. This helps to promote blood flow back to the heart. This specific pressure distribution is called “graduated pressure”. However, despite this benefit, many patients find them uncomfortable. This is especially true during warmer weather. Doctors traditionally recommended wearing compression stockings for up to six months for newly diagnosed patients. However, since 2013, NICE has suggested that patients should be referred directly to specialised vascular services. Although they can offer temporary relief, compression stockings do not address the underlying venous issues. 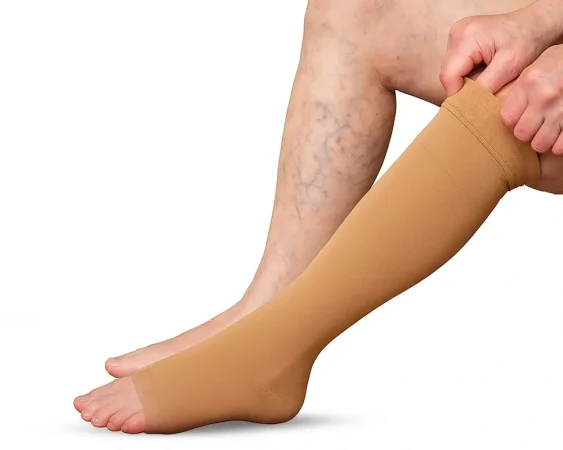
Treatment options aim to close or remove the damaged veins. One traditional method is "stripping," where the affected vein is surgically removed under general anaesthesia. However, prize-winning research from The Whiteley Clinic published in 2007 shows an important discovery. Stripping actually stimulates the body to grow new varicose veins back again after treatment. Since 2000, less invasive techniques have gained popularity. These are called endovenous thermal ablation, using either laser or radiofrequency. These methods destroy the vein from within using controlled heat. NICE guidelines recommend endothermal ablation as the first-line treatment for severe varicose veins causing pain or ulcers. If endothermal ablation is unsuitable or unavailable, foam sclerotherapy or surgery may be considered. Moreover, transitioning from surgery to newer methods could save the NHS around £400,000 annually. Yet, patients in some areas still receive outdated treatments as first-line options. In addition, costs for modern treatments can reach £5,000, compared to just £20–£90 for compression stockings.
Professor Gerard Stansby, a vascular surgeon at Freeman Hospital in Newcastle, stresses the need for better access to modern treatments. He notes that in many areas, obtaining advanced therapies or even surgery is nearly impossible. In the North East, NHS funding has allowed better provision of vascular treatments. However, elsewhere, patients often have to pay privately. Professor Stansby highlights the need for more training and investment in equipment for hospitals. This would ensure a successful transition to newer varicose vein treatments nationwide.
Professor Mark Whiteley, a consultant venous surgeon at the Whiteley Clinic, warns against viewing varicose veins as cosmetic. He highlights that untreated varicose veins can lead to a reduction in quality of life. Additionally, they can cause serious complications, such as blood clots, bleeding, and leg ulcers. Furthermore, Professor Whiteley believes compression stockings often delay proper treatments. Although compression stockings temporarily ease pain, they do not address the vein problem. Once removed, the underlying issue persists. Consequently, symptoms typically return. He criticises the reliance on stockings while proper treatments are delayed. Moreover, he raises concerns about NHS funding for advanced therapies. Without sufficient funding, patients may struggle to access modern treatments. Ultimately, effective treatment is crucial for long-term health, despite the temporary relief stockings offer. To read the full article, visit this link.