Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Lymphoedema is the swelling, usually of one or more of the limbs, due to poor or absent lymphatic drainage.
Although lymphoedema can affect other parts of the body, it is most commonly found in the leg followed by the arms.
Lymphoedema of the arms has become more widely known about in the public, due to the number of women having arm lymphoedema following breast cancer surgery or treatments. However, more people suffer from lymphoedema of the leg or legs but as this is a less well-publicised medical condition, it is often unknown about by the public.
The symptoms of lymphoedema relate mainly to the swelling of the limb.
Often, particularly in the early and mild lymphoedema, there are no symptoms. Patients often only notice it at all due to the swelling of toes or fingers followed by foot or hand.
If left untreated, and if it worsens, the limb may start to get quite heavy due to the extra fluid trapped within it.
At first, when the skin can still be dimpled with finger pressure, apart from the heaviness of the limb, there are often no other symptoms at all.
If the lymphoedema has come quickly, the skin can feel tense and inflamed. There can be a feeling of swelling of the limb.
If the swelling continues to increase, the limb can become very heavy and harder to move easily. If the lymphoedema has become chronic, the skin and underlying tissue can become quite hard and can start itching.
The two complications that must be looked at for our firstly cellulitis associated with lymphoedema and secondly, malignant change.
Fortunately cellulitis associated with lymphoedema is not too common, but once it happens once it can always happen again.
It has a classic course which should be recognised by doctors and nurses but is often not understood.
Because the lymphatic system is part of the immune system, when there is cellulitis associated with lymphoedema, the usual immune response to the cellulitis (which is an infection of the skin) is disordered.
Therefore in usual cellulitis, the leg or arm becomes red, hot and then tender and only after that does the patient start to feel unwell.
In cellulitis associated with lymphoedema, the usual cause is that the patient feels very sick often thinking they have flu. They often put themselves to bed. Thinking they have flu, they are usually surprised when 24 hours later the leg or arm with the cellulitis goes hot red and swollen.
Because the immune response is disordered, it usually means that antibiotics are needed for three weeks rather than the usual five days to one week. As such, patients are often given one week of antibiotics and when they don’t improve, often erroneously investigated for other problems such as diabetes.
Patients who have had one bout of cellulitis associated with lymphoedema should always make sure that they keep on top of the lymphoedema with manual lymphatic drainage (MLD) and also carry a supply of antibiotics around with them to start immediately on feeling unwell in the future.
Malignant change in lymphoedema is very rare but must be suspected if the limb with lymphoedema becomes hard, with red nodules appearing on the skin and often with itching. All patients with lymphoedema should really be under the care of a doctor or nurse with an interest in the condition. As such, any changes should be obvious to the healthcare professionals.
Manual lymphatic drainage (MLD) is a specialised form of therapy which is gentle and rhythmic. It is a technique which was developed in Europe in the 1930s by Emil Vodder. The method has now been adapted by medical professionals around the world to treat lymphoedema and there are a number of schools of MLD (including Asdonk and Földi in Germany, Casley-Smith in Australia, LeDuc in Belgium and Vodder in Austria).
The aim is to encourage protein reabsorption and stimulate lymphatic flow to improve drainage away from congested areas.
Manual lymphatic drainage (MLD) is a specialised form of therapy which is designed to improve the functions of the lymphatic system. The specific movements used in MLD treatments allow the superficial lymph vessels to reabsorb excess fluid, metabolic waste, large protein molecules and foreign substances from the tissues. The lymphatic fluid is then encouraged to empty into the deep lymphatic vessels and filtered through a series of lymph nodes along its route before it is returned to the blood circulatory system in the neck area.
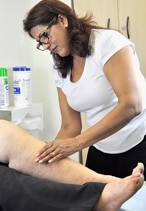 All patients with lymphoedema or at risk of developing it (for example after breast cancer surgery or after radiotherapy to the pelvis) can benefit from MLD.
All patients with lymphoedema or at risk of developing it (for example after breast cancer surgery or after radiotherapy to the pelvis) can benefit from MLD.
Apart from the relief or reduction in swelling and therefore improved comfort and quality of life, there is evidence that treatment also reduces the number of infective episodes and cellulitis. In addition, the skin and subcutaneous tissues often feel much softer after MLD.
Intensive Therapy comprises:
Complex decongestive therapy involves 2 to 4 weeks of:
Maintenance therapy comprises:
The Perometer is a very fast and easy way of measuring the volume of the limb. Within seconds the Perometer ring is slid up over the limb, and the exact dimensions are captured by the computer. This information not only allows us to keep an eye on how effective treatments are, but also to provide the most accurate way of getting the right stockings and bandages for our patients.

Sometimes tests would be performed to exclude other causes of leg swelling, for example, a scan of the veins in the leg (a duplex scan). Blood tests may be helpful in excluding other causes.
Often an isotope lymphogram or ‘lymphoscintography’ is used to confirm the diagnosis of lymphoedema. This test does not, however, show what type of abnormality is present, for example, too few lymphatics or a normal number of poorly functioning ones, but often this does not alter the management.
Very occasionally it is important to obtain a more detailed view of the lymphatics and this can be achieved with an operative lymphangiogram. A CT scan or pelvic ultrasound is sometimes performed when it is important to exclude a mass or lump in the pelvis or abdomen.