Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
A lesser-known venous anomaly first described in 2014, Primary Avalvular Varicose Anomalies (PAVA), may explain why some patients develop recurrent varicose veins despite receiving high-quality treatment. Originally identified by the research team at The Whiteley Clinic, this condition challenges conventional assumptions in venous diagnostics.
In this article, we explain what PAVA is, how it contributes to recurrence, and why recognising it is important for both clinicians and patients.
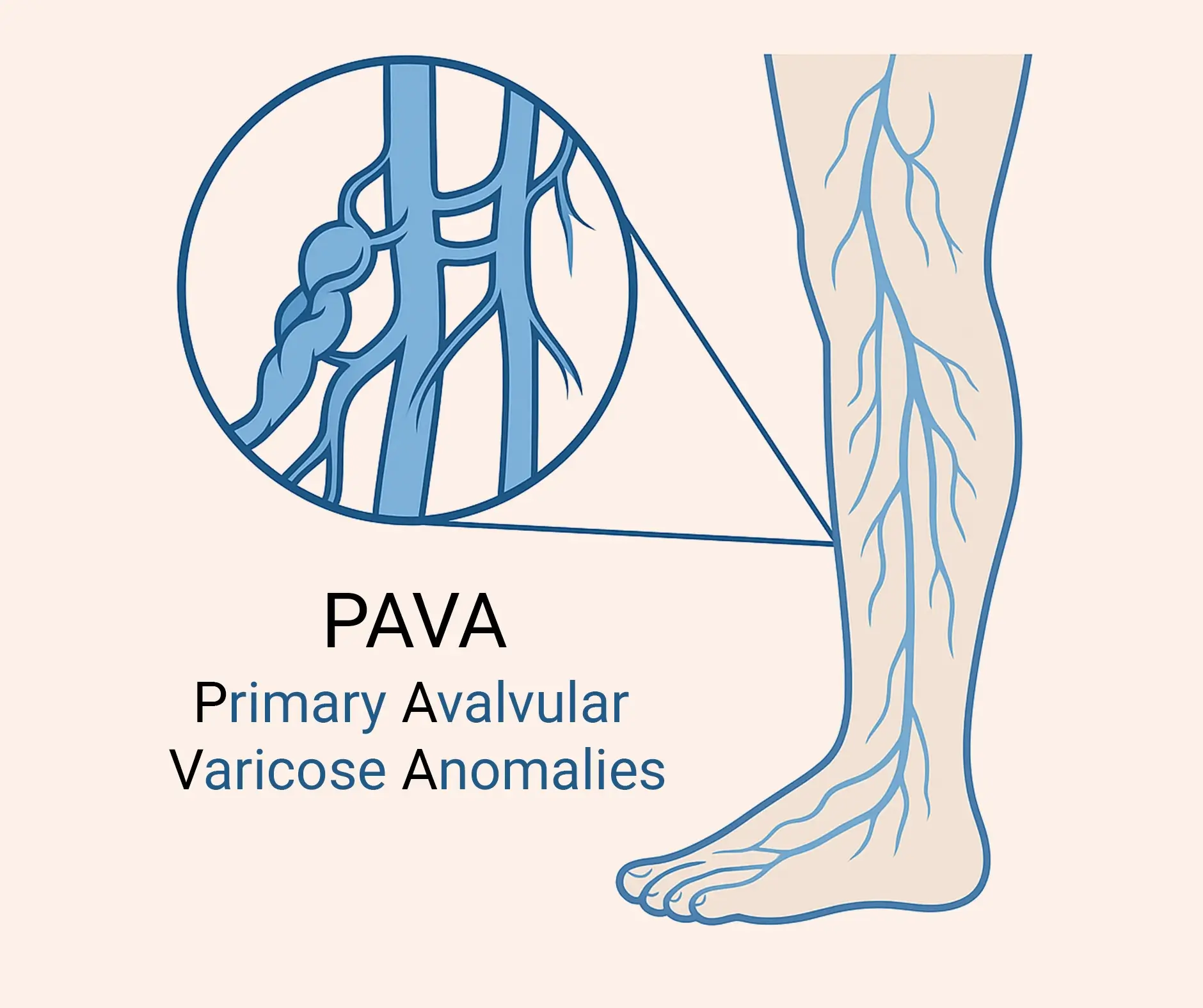
PAVA refers to small, thin-walled, serpiginous veins often found coiled around larger vein trunks in patients with primary varicose veins.
These vessels are unique because they have no valves at all.
Most varicose veins develop due to valve failure and venous reflux. However, these anomalies, in contrast, are avalvular from the beginning, which makes them structurally different right from the start.
Therefore, understanding this difference is vital for precise diagnosis and effective treatment.
In a study published in the Journal of Vascular Surgery: Venous and Lymphatic Disorders, researchers at The Whiteley Clinic discovered PAVA in 4.6% of legs examined from patients who had no history of surgery or trauma to the affected site. This data points to PAVA as a primary cause of varicose veins in a subset of patients.
You can Read the full study here.
PAVA often closely resembles neovascular tissue when viewed under duplex ultrasound. Consequently, many clinicians mistakenly interpret these vessels as new growth following previous treatments. However, this does not necessarily indicate true treatment failure. In fact, it often means that PAVA was present all along but, unfortunately, remained undetected prior to the initial intervention.
Therefore, detecting PAVA early is crucial to avoid misdiagnosis and improper management.
Researchers identified three main patterns of PAVA:
Recognising these patterns through detailed imaging is essential for precise diagnosis and treatment planning.
Interestingly, the study found that many women with Primary Avalvular Varicose Anomalies also showed signs of pelvic vein reflux. While further research is definitely needed, this finding nevertheless suggests a possible link between pelvic venous disorders and, consequently, the development of these avalvular anomalies. Moreover, understanding this connection could help guide more comprehensive diagnostic and treatment approaches in the future.
Treating PAVA often requires adjustments to standard varicose vein protocols.
For instance, when these anomalies are identified, clinicians may need to introduce additional therapies, such as foam sclerotherapy or ultrasound-guided ablation. These treatments would effectively complement conventional methods like endovenous laser ablation (EVLA).
To improve outcomes, specialists should therefore actively and carefully search for PAVA during pre-treatment duplex scans.
Without targeted imaging, there's a risk of missing these vessels, which could lead to repeated procedures that fail to address the true underlying issue.
The Whiteley Clinic has long been at the forefront of venous research, with Professor Mark Whiteley and his team pioneering a deeper understanding of complex venous conditions. Their landmark 2014 publication on Primary Avalvular Varicose Anomalies (PAVA) laid the foundation for improved diagnostic accuracy and more individualised treatment strategies.
Patients who suffer recurrence after vein treatments should consider seeking assessment from a clinic experienced in identifying advanced venous abnormalities. Clinics like The Whiteley Clinic incorporate recognition of PAVA into their standard diagnostic pathways, reducing the risk of misdiagnosis and unnecessary procedures.
Recognising PAVA before treatment is crucial, as it can prevent repeated procedures, significantly lower recurrence rates, and ultimately ensure more accurate and effective care. Moreover, as our understanding of venous disease continues to evolve, this important discovery by The Whiteley Clinic marked a turning point in our understanding of varicose vein recurrence and continues to influence modern diagnostic and treatment approaches.