Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Pelvic Congestion Syndrome (PCS) is a medical condition caused by internal varicose veins in the lower abdomen and pelvis, which cannot be seen on the surface. As with most names in medicine, the term Pelvic Congestion Syndrome is just a description of the problem itself.
Women suffering with PCS typically experience deep pelvic or uterine pain, which is often described as a heavy or dull ache, or often a “dragging” sensation. This pain often worsens throughout the day, particularly by prolonged standing or exercise. Women can experience sharp pains when they change their posture, walk, lift heavy objects, or engage in other activities that increase pressure on the abdominal area. Women suffering with PCS are also prone to painful menstruation and can experience deep discomfort during or following sexual intercourse. It can be so bad it can be a hindrance to having normal relationships. Research has shown that it can affect women who have never been pregnant, but it can also worsen with the number of pregnancies. In some cases, women with PCS will also experience urinary symptoms such as irritable bladder, urinary urgency, urge incontinence and an increased need to urinate during the night. One of the commonest signs of PCS are vulval or vaginal varicose veins. Many women who develop these varicose veins in intimate places, particularly after pregnancy, are told by their midwives or doctors that they cannot be cured and that they just need to wear tight pants. This is incorrect as these disturbing veins can now be cured permanently using our local anaesthetic procedures.
PCS is not taught as part of traditional training in gynaecology and so many gynaecologists do not recognise it. Hence most women who are suffering from the symptoms of PCS are not receiving the appropriate tests and treatments. Instead, they are either getting a misdiagnosis (usually being told they have “endometriosis”) or are put through expensive and less accurate tests such as MRI and CT and then told there is nothing wrong with them. Many women undergo unnecessary laparoscopy, which is performed under general anaesthetic and which has a risk of complications. Even after this, they are often told that there is nothing wrong with them as the pelvic varicose veins are not recognised as the cause of the problem. Research suggests that 1 in 3 (30%) women in the UK who attend gynaecology clinics with chronic pelvic pain suffer from PCS. However, it is not uncommon for these patients to receive misdiagnosis, misdirected therapies, or not to be offered any help at all.
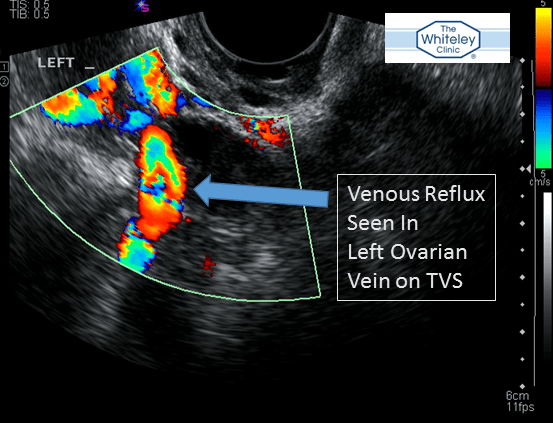
Ovarian vein reflux seen on Transvaginal Duplex Scanning - the best test for Pelvic Varicose Veins and part of The Whiteley Protocol for pelvic varicose veins
Research from The Whiteley Clinic has shown that the best way to look for pelvic varicose veins is a technique called transvaginal duplex ultrasound (TVS) using the Holdstock- Harrison technique. This technique was developed by Judy Holdstock, chief vascular technologist at The Whiteley Clinic. Judy and one of our other vascular technologists, Charmaine Harrison, developed the Holdstock-Harrison technique to diagnose pelvic vein reflux and this forms part of the Whiteley Protocol. Transvaginal duplex ultrasonography (TVS) as performed at The Whiteley Clinic is not widely available anywhere else in the world as it is a very complex technique developed at The Whiteley Clinic.
The Whiteley Clinic started treating pelvic vein reflux (PVR), the underlying cause of pelvic congestion syndrome in 1999. We were one of the first clinics in the world to start treating this condition and indeed there are now considerable numbers of publications in the peer-reviewed medical literature from The Whiteley Clinic. Pelvic Vein Embolisation is a process of using x-ray guided venography, planned by the results of the transvaginal duplex ultrasound, we can place very thin catheters directly into the veins that need treatment. Once the catheter is in place, a combination of foam sclerotherapy and insertion of a specialist platinum coil can be placed into the vein, closing it and stopping the pelvic vein reflux. Like our other treatments, PVE is performed under local anaesthetic as a walk-in, walk-out treatment at The Whiteley Clinic, Bond Street, London.
Pelvic congestion syndrome – chronic pelvic pain and pelvic venous disorders ISBN 978-1908586070
Although some patients are concerned about having coils placed into their pelvic veins, the actual metal involved is less than the clips used in many surgical procedures such as laparoscopic hernia repair or laparoscopic gallbladder removal and far less than the metal used in a hip replacement or other joint replacement procedure. Professor Whitley has written a book explaining pelvic congestion syndrome, the investigation and treatment “Pelvic congestion syndrome- chronic pelvic pain and pelvic venous disorders” If you are concerned you may have Pelvic Congestion Syndrome and would like to speak to an expert please call The Whiteley Clinic on 0330 058 1850 or email [email protected]