Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
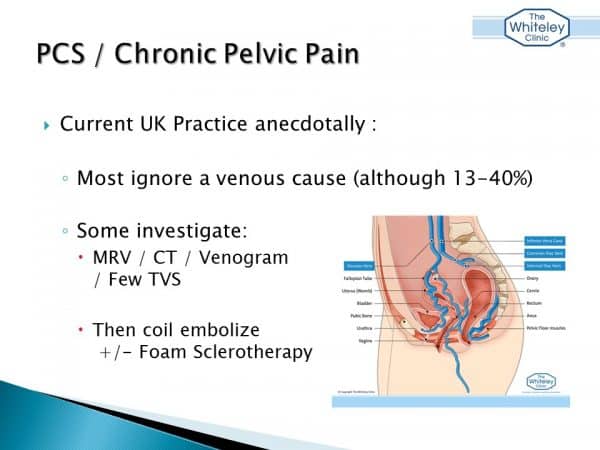
Chronic pelvic pain and pelvic congestion syndrome talk by Mark Whiteley - American Venous Forum Feb 2017
Pelvic pain that does not get better quickly, is called chronic pelvic pain (CPP). In approximately 13-40% of women with chronic pelvic pain, the cause of his pelvic venous congestion. This is also called pelvic congestion syndrome. Pelvic congestion syndrome can now be diagnosed with transvaginal duplex ultrasound scanning, performed using the Holdstock protocol. (see: https://thewhiteleyclinic.co.uk/diagnosis/transvaginal-duplex-ultrasound-scanning-tvs/) This was developed by Judy Holdstock of The Whiteley Clinic. Research has shown this is probably the best way to diagnose pelvic varicose veins which are the cause of pelvic congestion syndrome. (see: https://www.ncbi.nlm.nih.gov/pubmed/25324278)

Mark Whiteley speaking about pelvic congestion syndrome at The American Venous Forum - Feb 2017
Unfortunately, in the United Kingdom, and a lot of the rest of the world, doctors and nurses are not trained in diagnosing or treating pelvic venous congestion. The result of this is that even in the Royal College ofObstetricians and Gynaecologists Guidelines, the investigation of chronic pelvic pain does not include looking for any pelvic veins. Not surprisingly, it does not even mention any treatment of pelvic veins to get rid of chronic pelvic pain. Today Prof Mark Whiteley presented the current state of investigation and treatment of pelvic congestion syndrome in the UK. The research team at The Whiteley Clinic been specialising for 16 years pelvic vein reflux and pelvic congestion syndrome, and have many publications on this subject. Mark explained that most patients do not get investigated or treated as often left without a diagnosis. Mark and his team at The Whiteley Clinic have been involved in pulling together some research which is to be presented to the government at the College of Phlebology's 1st International Vein Meeting in London, on 16 March 2017. If you think might have public congestion syndrome, a good first self-assessment can be found at this link: https://thewhiteleyclinic.co.uk/self-assessment/pelvic-congestion-screening/
Live cases of Pelvic Vein Embolisation to be shown at College of Phlebology 1st International Veins Meeting 2017