Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
In 2013, the National Institute for Health and Care Excellence (NICE) approved endovenous or endothermal procedures as the recommended methods for treating varicose veins, including tortuous veins. This means that endovenous laser ablation (EVLA) and endovenous radiofrequency ablation (RFA) are now recognised as standard treatment options for both straight and tortuous varicose veins. All of these techniques involve the use of a catheter inserted into one of the two main superficial veins:
In addition, lasers, particularly EVLA, can be effectively used to treat smaller veins such as the Anterior Accessory Saphenous Vein, with proven efficacy. For years, the TRLOP technique has also been employed in the treatment of perforator veins in the calf and even the thigh.
Varicose veins naturally appear twisted and dilated. However, endovenous surgery targets deeper truncal veins—not the visible surface veins. Surgeons commonly target the Great and Small Saphenous Veins, and occasionally the Anterior Accessory Saphenous Vein. In most patients, these truncal veins are relatively straight, allowing the catheter to pass easily. However, if a patient has had prior complications, such as superficial thrombophlebitis or has suffered from varicose veins for an extended period, the vein walls may become significantly distorted, leading to the development of tortuous veins. In these cases, the vein develops kinks or bends, making catheter passage, particularly with a rigid catheter, more difficult. Once practitioners encounter tortuous veins, they choose the most appropriate treatment strategy.
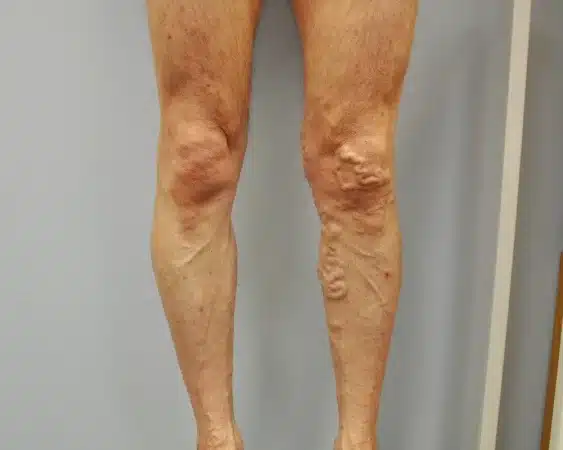
The Anterior Accessory Saphenous Vein rarely presents with tortuosity. The Small Saphenous Vein can be involved, but significant tortuosity is uncommon. If there is a history of thrombosis or scarring, other techniques may be applied, though tortuosity alone is usually not the main issue. However, the Great Saphenous Vein, especially in the thigh, is more prone to twisting. These techniques are therefore primarily relevant for treating veins in this area.
Tortuous veins are first detected via ultrasound imaging. A tortuous vein visible on the surface is essentially a varix, unless the patient is extremely thin, in which case the Great Saphenous Vein may be visible to the naked eye. Hence, during a diagnostic or intraoperative scan, tortuosity of the Great Saphenous Vein may be identified.
Regardless of the level of tortuosity, it is always worth initially attempting to advance the catheter, as it may naturally follow the curvature of the tortuous vein, straightening it during advancement. The procedure may begin either from below the knee or at the ankle, depending on the entry point of the catheter into the Great Saphenous Vein. The practitioner inserts the catheter under ultrasound guidance and advances it toward the tortuous veins. It is essential that the patient not lie completely horizontal. The bed should be tilted so that the head is raised to at least 15 degrees (reverse Trendelenberg position), helping the vein to dilate. If catheter progression is hindered in a supine position, the first step is to use the duplex ultrasound scanner to identify where the catheter is being blocked, and to see if simple catheter manipulation can help it advance.
If catheter advancement remains difficult due to tortuous veins, applying gentle pressure with a finger on the skin above the tortuous area can often help straighten the vein enough for the catheter to pass. If that fails, mobilising the leg, flexing the knee, lifting the leg at the hip, or rotating it slightly may improve catheter alignment. These manoeuvres should always be attempted prior to any attempt at catheter redirection. This type of limb movement must remain coordinated with the catheter tip at all times. Start by withdrawing the catheter slightly, then flex the patient’s knee and attempt re-advancement. If the catheter still does not pass, withdraw it again, elevate the leg further, abduct the hip, and try once more. In most cases, these manoeuvres allow successful navigation through the tortuous venous segment.
If the catheter still fails to progress through the tortuous veins, use ultrasound to locate the point of resistance. If the tip needs to angle downwards, apply pressure from the skin surface just above the tip. There's no need for guidewires as finger pressure alone can often steer the catheter in the desired direction. Apply light pressure on the side you want the tip to move towards. To lift the tip upwards, move approximately 10 cm back along the catheter and apply pressure; this typically redirects the tip toward the probe, enabling successful advancement. 👉 Watch this demonstrated in the video by Professor Mark Whiteley:
In this College of Phlebology video, Professor Mark Whieley describes different methods to get around this problem. A tortuous vein should never be the cause of a failed endovenous operation and should never stop doctors from treating varicose veins with endovenous laser or radiofrequency.
If these techniques still do not permit catheter passage through the tortuous segment, identify the next accessible straight portion of the vein and create a new entry point there. Treat that section as a separate segment. Use EVLA or radiofrequency to treat the vein up to the tortuous point. Then, from a higher access point, continue treatment. The tortuous section itself can later be treated using ultrasound-guided phlebectomy or foam sclerotherapy.
Skilled practitioners rarely fail when using these minimally invasive approaches. If you master ultrasound-guided vein access, you can re-enter the same vein multiple times—two, three, or even more. You can then treat each segment using laser or radiofrequency, and remove or sclerose the sections in between when necessary.
Treating tortuous varicose veins with EVLA or RFA marks a major advancement in modern vein care. As a result, more patients now benefit from less invasive procedures. Ultrasound imaging quickly detects tortuous veins before treatment begins. Then, skilled practitioners use precise catheter navigation to target the problem areas. This step plays a key role in achieving successful outcomes. In addition, choosing the best treatment strategy improves safety and results. Flexible, fine-tip catheters easily follow the curves of affected veins. Proper patient positioning also supports smoother catheter movement. Moreover, small manual adjustments, like leg movement or finger pressure, can guide the catheter through tough spots. Together, these techniques reduce complications and increase the effectiveness of the procedure. At The Whiteley Clinic, experts first carry out a detailed assessment for every patient. Based on the results, they select the most suitable treatment approach. As a result, each patient receives a plan tailored to their specific vein condition. This personalised care helps achieve the most effective and lasting outcome.