Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Haemorrhoids and Varicose Veins may appear to be unrelated conditions, but modern research is revealing a surprising connection. Both may stem from faulty venous valves and blood reflux, particularly in the pelvic region. This link not only changes the way we view haemorrhoids but also how we treat them, moving beyond traditional surgery to targeted venous care.
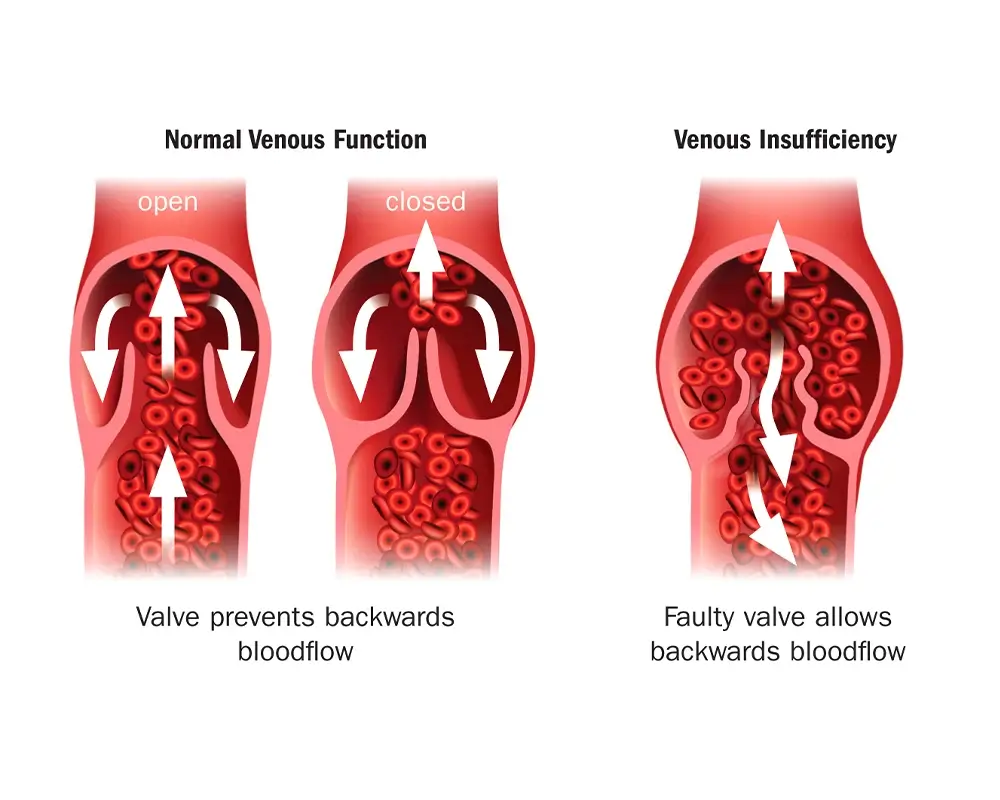
While often attributed to straining during bowel movements, pregnancy, or a low-fibre diet, haemorrhoids may also be a sign of deeper venous issues in the pelvis.
Some symptoms of haemorrhoids, particularly in women, overlap with those of pelvic congestion syndrome (PCS), a condition caused by pelvic varicose veins. PCS symptoms include:
This overlap has led researchers to ask whether haemorrhoids could, in some cases, be a local manifestation of pelvic venous reflux, part of a broader disorder involving Haemorrhoids and Varicose Veins.
One of the pioneering researchers to explore this connection was Professor Mark Whiteley.
In 2014, he published findings suggesting that many patients with haemorrhoids also have pelvic varicose veins.
To diagnose this, Professor Whiteley uses a specialised transvaginal or transrectal duplex ultrasound scan. This scan allows vascular technologists to examine deep pelvic veins in detail, identifying any faulty valves or refluxing blood flow. This diagnostic step is crucial because standard leg scans often fail to detect pelvic vein problems.
By accurately detecting the source of the reflux, clinicians can offer a more effective and lasting treatment, rather than simply removing the haemorrhoid without addressing the underlying issue.
To hear Professor Whiteley's full explanation of the connection between haemorrhoids and varicose veins, you can watch his detailed video presentation here:
In his 2014 video presentation, Professor Whiteley described a pivotal moment when a patient asked whether his haemorrhoids were part of his varicose veins. Although he initially said no, further research led him to reconsider.
By using duplex ultrasound imaging, the team found a consistent link between haemorrhoids and pelvic vein reflux. The conclusion was clear: Haemorrhoids and Varicose Veins could belong to the same venous disease family.
This was a major shift in understanding. Traditional treatments—like haemorrhoidectomy or artery ligation—may address only the symptom rather than the underlying cause. If the real issue is refluxing blood from the pelvis, treating that reflux could prevent recurrence and reduce symptoms more effectively.
Since that early research, more data have emerged to strengthen the case:
A study involving 31 million people found a strong bidirectional association between Haemorrhoids and Varicose Veins, showing they often co-exist and may share common risk factors like valve failure and increased venous pressure.
New data show that medications can reduce symptoms of pelvic congestion syndrome and may help in managing pelvic-related haemorrhoids.
Pelvic vein embolisation, a minimally invasive procedure that blocks refluxing veins, has shown to significantly improve haemorrhoid symptoms in patients with confirmed pelvic vein issues.
Given the evidence, clinicians should consider:
This integrated approach is showing promising results for those suffering from both Haemorrhoids and Varicose Veins.
The association between Haemorrhoids and Varicose Veins is no longer just a theory. It is now backed by imaging, clinical outcomes, and global research. As a result, we must rethink how haemorrhoids are classified and treated—especially in patients with pelvic symptoms. This approach consequently leads to more effective and sustained treatment for patients.
If you experience haemorrhoid symptoms along with leg or pelvic vein issues, the two may be more closely related than you think.
To learn more about this significant discovery, watch Professor Whiteley’s video from 2014, and then seek advice from a vein specialist on current diagnostic options.
Haemorrhoids and Varicose Veins may share a common vascular origin, so it’s essential to consider them together for effective treatment.