It amazes me how many people claim to have suffered from phlebitis as the term is often over used by the public and more worryingly by nurses and doctors.
To make this clear, it is important to understand that
phlebitis does not mean just any pain or inflammation in the lower legs, which is what many believe.
Why this is a problem
Like most medical conditions phlebitis poses no threat if you do not have it! Recent research into phlebitis and other venous conditions shows that in some patients the condition can be very serious indeed, making it all the more important for a proper diagnosis. Treatment may require the sufferer to take anticoagulation drugs, commonly rivaroxaban, warfarin or heparin which is used to prevent deep vein thrombosis (DVT). There is also risk of a clot to the lung which can be life threatening. Doctors and nurses who do not specialise in the venous field do not fully understand phlebitis and often mistreat their patients by prescribing antibiotics, which have no effect on the condition whatsoever.
What is phlebitis and how is it treated?
To put it simply, phlebitis is when the vein develops an inflammation.
If you have been recently hospitalised and have had a drug injected or a drip placed into your veins, then virtually all occurrences of phlebitis will be in the veins of the legs.
The cause of the inflammation in the veins is due to blood clots. We are not talking about the deep veins here, as this would be the dangerous deep vein thrombosis (DVT). These are clots in the superficial veins which lie just beneath the skin; this condition is known as superficial venous thrombophlebitis (SVT).
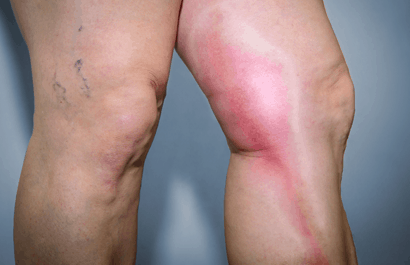
In most cases phlebitis always occurs in varicose veins, even the ones that cannot be seen as they are under the surface of the skin. We refer to these as “hidden varicose veins”. The structure of the vein is tubular and typically sufferers of the condition usually feel a lump in the leg under the skin. The clot in the vein causes inflammation in the vein wall and the surrounding area becomes red and hot. We can understand why doctors and nurses prescribe antibiotics here, and this is because typically anything which is red and hot on the skin indicates an infection, such as cellulitis for example.
Phlebitis should only be diagnosed if there is a tender lump or area in the leg where a vein runs, remember you might not be able to see this vein. Brown or red coloured skin around the ankle and/or a swollen and tender calf with redness spreading up the leg are often seen in other conditions but not in phlebitis.
Up until just recently when doctors and nurses diagnosed phlebitis the treatment path was to prescribe an anti-inflammatory pain killer like aspirin, which would be taken regularly, as this would reduce the inflammation and the pain. Support stockings would be used to provide relief in the affected area and to make sure that the blood flowed properly to the other veins, which in turn would reduce the risk of clots elsewhere.
Over the last few years, reports of patients diagnosed with DVT and clots in the lungs from superficial thrombophlebitis or clots in the superficial veins, have seen two very influential committees review and subsequently change their guidelines on how to diagnose and treat phlebitis. The British Committee for Standards in Haematology and the American College of Chest Physicians have both produced guidelines which now grade the risk of the phlebitis and recommends different treatments depending on the individuals risk. Tailored treatments might be the use of oral blood thinning medications such as warfarin, heparin injections for a couple of weeks or in more minor cases non-steroidal anti-inflammatory painkillers and support stockings. The guidelines have been put into place to prevent patients with phlebitis progressing to a dangerous DVT or worse.
This is all very well of course and assumes that the diagnosis by the doctor or nurse is correct. When diagnosing the doctor or nurse needs to know that the “phlebitis” is definitely superficial venous thrombosis, and secondly whether or not the clot causing the problem is isolated in a vein just under the skin or whether it has already extended along the vein or even deep into the deep venous system within the muscle. There is only one sure fire way to confirm the presence of a clot in the vein and to measure the extent of the condition and that is to perform a special venous test known as a venous duplex ultrasound scan.
This test is now widely available in specialist veins clinics and hospitals so patients should be able to have the necessary scans to correctly diagnose phlebitis.
How to avoid misdiagnosis
It is now the case of educating both patients to understand the symptoms of this condition and healthcare professionals to know that a diagnosis of phlebitis requires an urgent venous duplex ultrasound scan both to confirm the diagnosis and to plan the correct treatment which will reduce the risk of complications from the superficial blood clot in the leg.
