Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Phlebitis is often misdiagnosed and mistreated. Today a patient came to The Whiteley Clinic for a second opinion and got some shocking news.
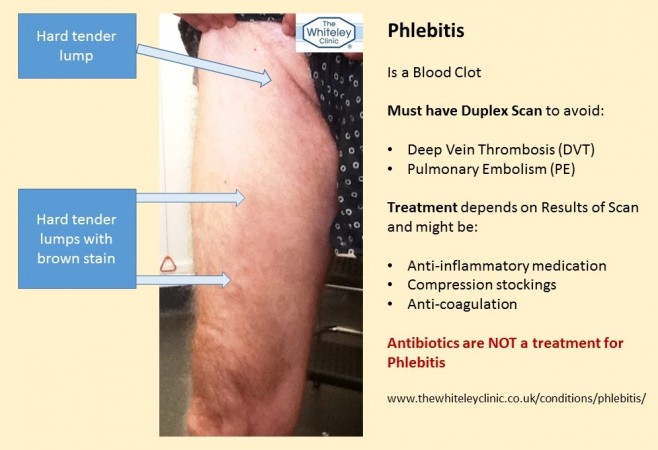
Phlebitis - Having a Duplex Scan may save your life - Treatment for Phlebitis is not antibiotics
The patient knew he had varicose veins. He had seen them on his legs for several years. He had not had his veins treated as they were not troubling him and he did not know varicose veins can lead to serious complications without any warning symptoms.
Three years ago he had a long haul flight. A day or two later he had a tender lump just above his right knee. His doctor gave him anti-inflammatory gel to rub onto it and did not give him a diagnosis. The lump and tenderness took a very long time to settle and the lump never completely disappeared.
Three months ago, the patient had a sudden kidney stone. He was admitted and given very strong pain killers. The kidney stone pain settled. However over the next day or two he noticed a hard tender lump all of the way up his thigh towards the groin. He cold even feel two lumps in the groin itself. His doctor told him he had phlebitis. He gave him more anti-inflammatory gel, some antibiotics and sent him for an ultrasound scan to the hospital. A quick scan there diagnosed "Two veins - a large one and a small one". He was told nothing more needed doing.
Fortunately the patient called The Whiteley Clinic for a second opinion. It would have been much better if he had called 3 months before. Following The Whiteley Protocol®, the patient was seen by a consultant specialising in venous disease. He was then scanned by a The Whiteley Clinic trained specialist vascular technologist using a top of the range duplex ultrasound scanner. This scan showed there was superficial thrombophlebitis - blood clot - filling the 2 major superficial veins in the thigh. These are the Great Saphenous and the Anterior Accessory Saphenous Veins. More importantly, the clot extended into the groin and was bulging into the deep vein (the femoral vein).
Research has shown that blood clot or phlebitis in the superficial veins of the leg can lead to DVT and can even go to the lungs - a Pulmonary Embolism (PE). These risks are high enough that guidelines have been published from the USA and the UK in 2010 and 2012 that said:
Please note:
So how does this affect this patient. The patient should have had a scan 3 months ago and should have been anti-coagulated. Fortunately he does not seem to have had a pulmonary embolism in that time. As such, the patient has now been recommended to have anti-coagulation until the clot is gone and the risk is reduced. At that point, we need to treat the varicose veins to stop the phlebitis and all of the risks from returning again.