Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Varicose veins occur because the valves in the leg veins stop working or fail. The result of this is that when patients with varicose veins stand up, blood in their leg veins falls down to the ankle, causing an impact pressure on the veins lower down in the legs. The column of blood from the heart to these veins is heavy, stretching the vein wall and hence causing varicose veins. We have already discussed this in CEAP C2 disease.
The next worse classification after simple varicose veins is CEAP C3 – Swollen ankles (also known as oedema) due to the varicose veins. As this is a clinical classification, the swollen ankles should be seen in legs that have clear varicose veins. Of course we know that for everybody who has visible varicose veins, there is another person who has “hidden varicose veins”. In these patients with “hidden varicose veins”, the same valves have failed causing venous reflux, but the veins near the surface have not dilated. The result of this is the same internal problem with blood falling the wrong way down the veins, but no visible varicose veins.
In these cases, where there is swelling of the ankles (ankle oedema) and no obvious varicose veins visible on the surface, this really should not be called CEAP C3 as it is not a clinical diagnosis of venous oedema secondary to varicose veins. However, if we have proof that there is venous reflux using duplex ultrasound, and swelling of the ankles, it is quite right to classify this as CEAP C3 to be correct, rather than be pedantic and not use this classification.
As CEAP C3 is physical damage due to inflammation from the varicose veins and venous reflux, this is clearly worse than the C2 disease where there is no damage to the tissues surrounding the varicose veins. Therefore it is not surprising that in the UK the NICE (National Institute of Health and Clinical Excellence) and elsewhere in the world other regulatory bodies, suggest that C3 is a medical condition that should be funded for treatment.

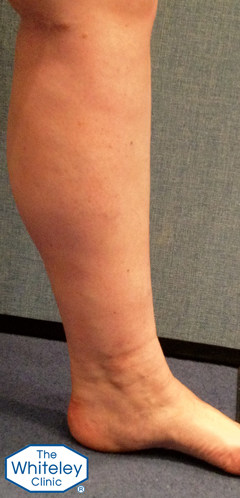
Swollen ankle with varicose veins and stock imprints – CEAP C3
So what is actually seen when you examine yourself or someone whom you suspect to have CEAP C3 disease?
Firstly there should be varicose veins visible, although as you will see from above, this might not be the case if the venous reflux is due to “hidden varicose veins”.
Secondly, there should be swelling of the ankles. Although this would appear to be obvious, there are certain points to this swelling that are well worth knowing.
Swelling of the ankles due to varicose veins, or venous oedema, usually affects the leg underneath the calf and around the ankle bones. It rarely extends onto the foot itself and does not extend to the toes. If the foot and toes are grossly swollen, this is almost always lymphoedema or other generalised oedema and not venous oedema. Therefore patients or people with swelling of the ankles, feet and toes should not be diagnosed as CEAP C3 and the cause of the swelling should not be assumed to be varicose veins or venous reflux, without specialist assessment.
In most cases, the swelling is probably less than you would imagine. In the mornings, when you first wake up, the swelling from CEAP C3 venous oedema is rarely noticeable. This is because when you have been lying down for several hours, there has been no venous reflux as the valves have not been needed to act as antigravity devices. Hence blood flow from the legs has been normal and there has been no build up of fluid at the ankles.
After getting up and starting the day, venous oedema will start to form as the day progresses. The speed at which it forms depends on several things including the severity of the varicose veins or hidden varicose veins (venous reflux), how active you are and what you are doing (i.e. standing, sitting, swimming et cetera). Generally, as the day progresses some swelling occurs at the ankles. This is usually only noticed by the imprint of socks at the ankle when they are removed. If the swelling is huge and makes the socks tends cause the foot to swell inside a shoe, once again one should suspect other causes of swelling including lymphoedema. The swelling of CEAP C3 venous oedema is usually more subtle than you might expect.
There are a couple of possible causes for the swelling found in CEAP C3 disease from varicose veins. These causes may well be linked. As noted above, varicose veins or “hidden varicose veins” (venous reflux) occurs because the valves in one or more of the leg veins fail. On standing, blood tries to fall with gravity back towards the ankles down the veins. In normal people, the valves close, stopping the backward flow or “reflux” of the venous blood.
If the valves in any of the veins have failed or have stopped working, blood falls back down the veins by gravity. This ends up with a column of blood that may stretch from heart all the way down to the ankle. The pressure on the vein wall at the bottom of this column of blood can be very high, forcing fluid from the blood out through the vein wall and into the surrounding tissue.
Research has also shown that there is inflammation in the blood within the veins when there is venous reflux. Therefore another possible cause is that when the blood falls down the veins, it hits the vein at the ankle, causing inflammation. One of the consequences of inflammation is swelling. You will know this from any time you have bumped yourself – the area goes hot, red, swollen and is painful. Not surprisingly, in CEAP C3 disease, the ankle is swollen and is often a little redder, warmer and can quite often ache. This suggests that inflammation may be involved rather than just pressure of the column of blood.
Our research has also suggested other reasons why inflammation might be involved but that is probably beyond the scope of this webpage.
If you are interested in this subject and want to read more, please see the book Understanding Venous Reflux – the cause of varicose veins and venous leg ulcers.
If you suspect that you have CEAP C3 swollen ankles due to varicose veins, it is essential that you have a venous duplex ultrasound scan performed by a specialist vascular Scientist to identify whether the swelling is due to venous reflux. Although many doctors performing their own scans may be able to see reflux in the big veins such as the great saphenous vein and the small saphenous vein, only specialist centres with specialist vascular scientists specialise in venous duplex ultrasound scans will be able to regularly and accurately diagnose the less well-known causes of venous reflux, such as perforator vein incompetence, pelvic vein incompetence and isolated deep vein incompetence.
In addition, it is essential that the deep veins are examined in detail as swelling can also be due to obstruction or partial obstruction of the deep veins rather than just reflux. To get the correct treatment it is important to know the difference between these two conditions particularly as they can coexist.
In the past, family doctors and general practitioners, district nurses, the NHS and private medical insurers have suggested that if you have swelling of the ankles due to varicose veins (CEAP C3) you should have graduated compression stockings or surgical support stockings to try and treat this.
However, research has shown this to be untrue as graduated compression stockings or surgical support stockings only provide any improvement whilst they are being worn. They do not alter any of the problems of the venous reflux causing the varicose veins or “hidden varicose veins” and so never cure this condition. Graduated compression stockings or surgical stockings should only be worn for symptomatic relief whilst proper investigations and treatment are instigated, or in the post-operative period support might be required after endovenous laser ablation, radiofrequency ablation, foam sclerotherapy or other treatments have been performed.
Once the venous duplex ultrasound scan has been performed, any fluid around the ankles (venous oedema) will have been seen on the duplex ultrasound scan as fluid shows up very clearly. In addition, any venous reflux will also have been identified if the scan has been performed by a specialist vascular scientist. The level and amount of reflux and the amount of oedema can then be assessed by a specialist in vein surgery to check that they correlate. If they do, a diagnosis of CEAP C3 venous oedema due to varicose veins can be confirmed.
Although it is not essential to operate if the patient does not want to, failure to treat this condition will almost always lead to further deterioration and worsening of the signs and symptoms. Unless the patient is particularly unwell or there are other extenuating circumstances, almost every venous expert in the world would suggest that the venous reflux is stopped by treating the varicose veins or “hidden varicose veins”. The treatment used will depend upon the pattern of reflux and may include:
A combination of these methods is usually highly successful in reversing the venous reflux and getting rid of both the ankle swelling as well as the varicose veins or hidden varicose veins.