Klippel-Trenaunay Syndrome (KTS)
March 26, 2026
Varicose veins is the clinical diagnosis of bulging veins in the legs. They can be fairly easily diagnosed clinically as they bulge when the patient stands up and then disappear when the patient lies down and elevates the legs
Approximately 15 to 20% of the adult population in Western countries have these visible varicose veins. Interestingly another 15 to 20% have hidden varicose veins that cannot be seen on the surface. However, as the CEAP clinical score is only associated with what can be seen on the surface, hidden varicose veins will not be discussed here.
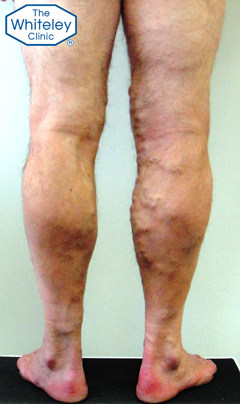
Severe Varicose Veins in a man – CEAP-C2
The bulges of varicose veins on the legs can extend anywhere from the buttocks and groin areas, all the way down to the feet.
Commonly, varicose veins are seen in the calf and lower leg. If there are discoloured patches around the ankles, this is not simple CEAP C2 varicose veins but will become skin damage and therefore CEAP C4 skin damage.
Varicose veins of the legs bulge on standing and disappear on lying down, particularly if the leg is elevated and if the varicose veins are relatively deep, then the skin overlying the vein bulges as well, but the dark colour of the blood cannot be seen through the skin. In these cases, the bulges are coloured.
If however the veins are near the surface of the skin, then it can be possible to see the deoxygenated blood in the veins through the skin. When this happens, the bulging varicose veins can look green or even bluish purple. Of course, when the legs are elevated, blood flows out of the varicose veins and so the colour disappears, as do the bulges.
The distribution of the bulges can help doctors understand where the veins are coming from. Most importantly, if the bulges are around the tops of the thighs, buttocks, perineal area or near the vulva and vagina in women or top of the scrotum in men, then this may be a sign that the varicose veins are not simple leg varicose veins but arise from pelvic vein reflux.
In these cases, it is essential that the pelvic veins are investigated and treated if necessary to stop varicose veins coming back again in the future.
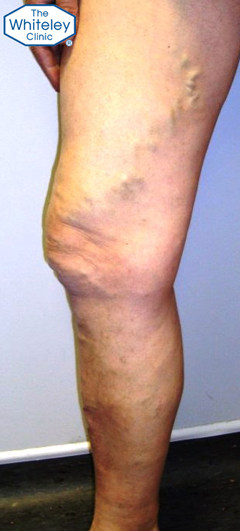
Thigh and calf varicose veins – CEAP-C2
In the vast majority of cases, varicose veins of the legs (and pelvis) are caused by the failure of valves in the veins. Veins pumps blood back to the heart and so have to pump blood up against gravity. Movement of the muscles in the legs cause the blood to be pushed upwards inside the veins. In most people, blood cannot then fall back down the veins because valves close preventing this from happening.
In people who suffer from varicose veins, these valves give way and allow blood to fall back down the veins. This is called venous reflux. The blood falling back down the veins can damage the skin around the ankle and lower leg. To try and stop this from happening, the body makes “shock absorbers” to try and direct the falling blood away from the veins at the ankle. These dilated veins that act as “shock absorbers” are varicose veins.
It is because the varicose veins fill with blood falling back down the veins with gravity, that varicose veins are tense and bulging on standing. Similarly when the legs are elevated, blood falls with gravity back up the veins towards the heart and the varicose veins disappear by emptying.
Doctors used to be taught that leg varicose veins can be caused by blockages of the veins in the pelvis such as by pelvic tumours, pregnancy, constipation, obesity and other things that raise the pressure in the abdomen. However, if varicose veins were really caused by blockages of the pelvic veins, then they would not only bulge on standing but would also continue to bulge on lying down as the blood would not be able to flow out of the leg.
We now know that when the pelvic veins are blocked, the result is not simple varicose veins but can be a combination of some swollen veins in addition to swollen, tender, warm and often discoloured legs.
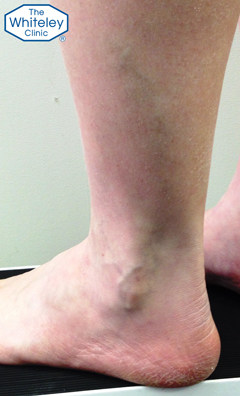
Varicose Veins of the outer lower leg and lateral ankle – CEAP-C2
One option if you have varicose veins is to do nothing. Many people with varicose veins do nothing until they get worse and start causing worse symptoms or complications. However, leaving varicose veins without doing anything will result in them deteriorating and getting worse. This might be a slow process, or may be very fast, particularly if a clot forms within them. See our page on phlebitis for more information. Indeed a research study in 2006 showed that if uncomplicated varicose veins were left untreated, the patients had a worse quality-of-life after two years than if they were treated surgically.
www.ncbi.nlm.nih.gov
If you have varicose veins and do not have a scan, then it is impossible to know how severe the underlying venous reflux disease is. Having a duplex ultrasound scan performed by a specialist clinic, will inform you of the underlying venous problem and will allow you to decide along with your specialist, whether it is safe to leave your varicose veins for the time being or whether it is sensible to get them treated.
Hence, if you have varicose veins it is essential to have a venous duplex ultrasound scan performed by a specialist who performs venous duplex ultrasound scan every day. At The Whiteley Clinic we only allow these venous duplex ultrasound scans to be performed by The Whiteley Clinic trained vascular scientists. Research has shown that when doctors do their own scans, unless they do nothing but scanning for other doctors, they usually miss many of the underlying causes of varicose veins. Therefore, the national guidelines are that doctors should work in teams with other professionals that are able to provide a full duplex examination and are able to perform all the vein treatments that might be needed.
The venous duplex ultrasound scan should look at all of the veins in the legs to find out which ones are working normally and which ones are not. This should include all of the superficial veins, the truncal veins, the perforator veins in both lower and upper leg as well as all of the deep veins to make sure there are no deep vein problems such as an old deep vein thrombosis or deep venous reflux.
If there are any varicose veins around the buttocks, perineum, vulval or vagina in a woman or scrotum in a man, then further examination of the pelvic veins is essential to find out if the varicose veins actually come from the pelvis. Research from The Whiteley Clinic shows that if this is missed, and only the leg varicose veins are treated, this can be a major cause for varicose veins coming back again in the future after treatment.
See our published research here: Pelvic Varicose Veins Are A Major Cause Of Recurrent Varicose Veins
In addition to the venous duplex ultrasound scan, another test called a photoplethysmography (PPG) can also see how severe any venous reflux is. For a full explanation, follow the link within this paragraph.
The treatment of varicose veins is very complex because there are so many different causes of varicose veins.
The principles of good treatment are the basis of The Whiteley Protocol®.
The general principles of varicose vein treatment are: